Degenerative Disc Disease
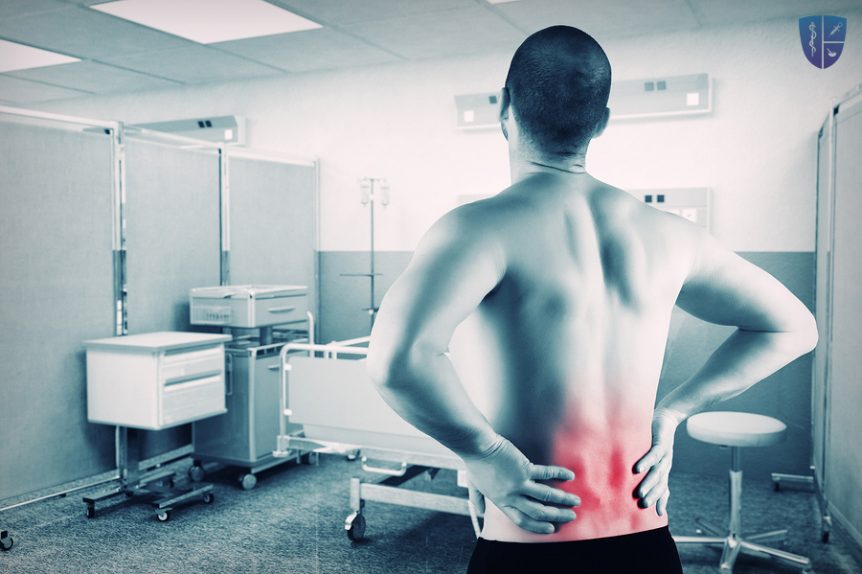
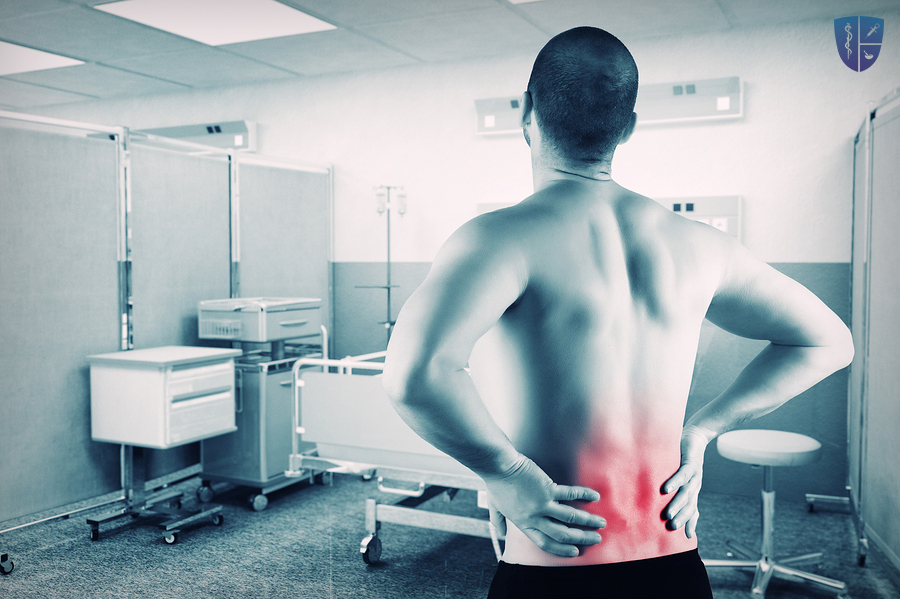
Degenerative Disc Disease is the formal name for the degeneration or normal wear on the intervertebral discs. Though each patient’s level of pain will vary, degenerative disc disease (DDD) is frequently the cause of low back pain, especially in young adults. Painful disc degeneration is common in the neck (cervical spine) and lower back (lumbar spine). These areas of the spine undergo the most motion and stress, and are most susceptible to disc degeneration. Some patients do not experience any pain at all. Those who do have pain usually have experienced an acute injury to the disc that resulted in some instability of the spine and inflammation. As the healing process progresses, the instability is corrected and the incidents of pain become less frequent. Some other associated symptoms include numbness, tingling and pain radiating into the extremities. If weakness develops or symptoms worsen, DDD might have progressed into a disc herniation.
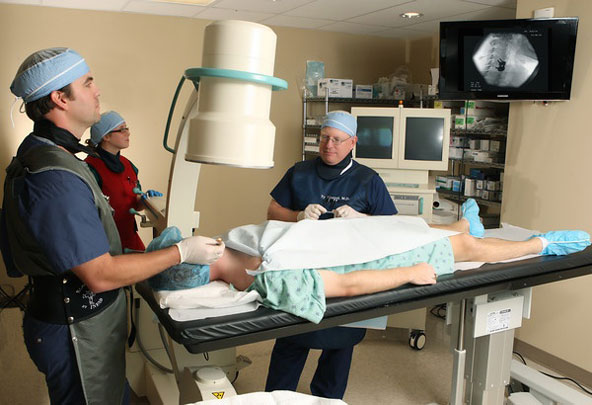
A physician will collect a medical history, perform a physical exam and order an imaging study like a MRI. However, MRI results are not sufficient evidence to diagnose DDD.
DDD can be treated by exercise and physical therapy to build strength and stability, activity modification and application of ice and heat to the area. For mild cases, over-the-counter non-steroidal anti-inflammatories (NSAIDs) or pain relievers will be suggested. A short-term opiate prescription may be considered for severe pain. If conservative treatments fail, many surgical options exist. About 65% of patients experience improvement after surgical intervention.
Overview
This condition is a weakening of one or more vertebral discs, which normally act as a cushion between the vertebrae. This condition can develop as a natural part of the aging process, but it may also result from injury to the back.
Disc Wall Tears
Degenerative disc disease typically begins when small tears appear in the disc wall, called the annulus. These tears can cause pain.
Disc Wall Heals
When the tears heal, creating scar tissue that is not as strong as the original disc wall. If the back is repeatedly injured, the process of tearing and scarring may continue, weakening the disc wall.
Disc Center Weakens
Over time, the nucleus (or center) of the disc becomes damaged and loses some of its water content. This center is called the pulposus, and its water content is needed to keep the disc functioning as a shock absorber for the spine.
Nucleus Collapses
Unable to act as a cushion, the nucleus collapses. The vertebrae above and below this damaged disc slide closer together. This improper alignment causes the facet joints – the areas where the vertebral bones touch – to twist into an unnatural position.
Bone Spurs Form
In time, this awkward positioning of the vertebrae may create bone spurs. If these spurs grow into the spinal canal, they may pinch the spinal cord and nerves (a condition called spinal stenosis). The site of the injury may be painful.
Symptoms
Some people experience pain, numbness or tingling in the legs. Strong pain tends to come and go. Bending, twisting and sitting may make the pain worse. Lying down relieves pressure on the spine.
Schedule your appointment today and meet with our providers to discover if this treatment is right for you.