Diabetic Peripheral Neuropathy involves the peripheral nervous system (PNS). While the central nervous system (CNS) includes your brain and spinal cord, the PNS includes all of the nerves that start in your spinal cord and innervate the rest of the body. Peripheral neuropathy can be caused by vitamin deficiencies, alcoholism, autoimmune diseases, some medications, diabetes and other unknown causes. Damage to the PNS can cause nerves to function improperly causing numbness, tingling or pain.
Two main types of diabetes exist: Type I, or Insulin Dependent, and Type II, or non-Insulin Dependent Diabetes Mellitus. Committing to a well-balanced diet and exercise regimen are the two most important factors in managing diabetes. If the patient’s blood sugar levels are not controlled by diet and exercise, medications may be required. Lack of control over the blood sugar level leads to the complications associated with diabetes.
Neuropathy in general can be difficult to diagnose. A physician will collect a thorough medical history and perform a physical exam. The doctor may also order certain lab tests to rule out vitamin deficiencies. Nerve conduction studies or electromyography (EMG) may help with the diagnosis.
Treating diabetic peripheral neuropathy can be harder than diagnosing it. The physician’s main treatment goals will be to control blood sugar levels and manage the related symptoms. Due to the complexity of this type of pain, the doctor may have to try several different approaches before finding one that is effective.
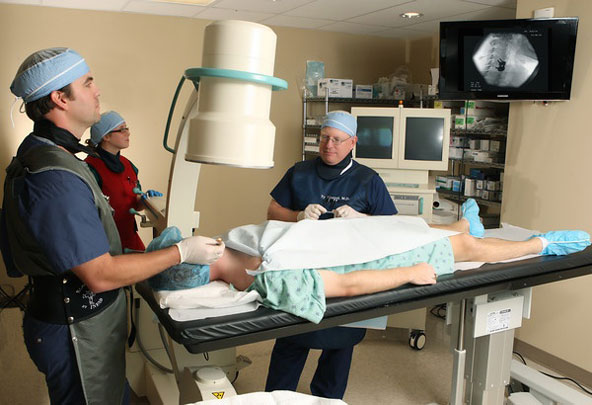
Therapies that might be beneficial include spinal cord stimulation, vitamin/nutrient therapy and alternative therapies such as acupuncture and biofeedback. Membrane stabilizing medications such as Cymbalta, Lyrica, Neurontin and Tramadol may be used for calming irritated nerves. Opiate pain relievers may offer some relief, but opiates are not usually used for this type of pain.